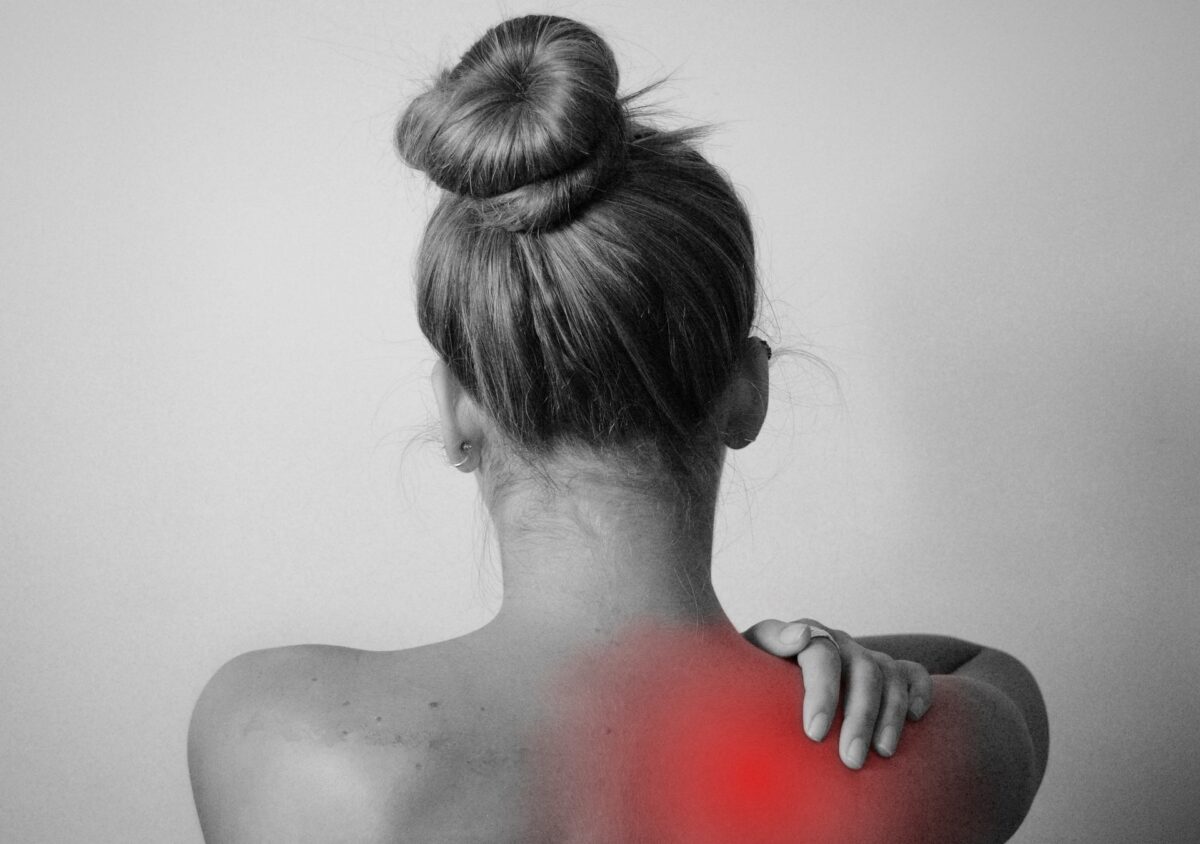
If you suffer from fibromyalgia, you know that it can be a debilitating condition that causes fatigue, pain, insomnia, gastrointestinal issues and brain fog. There is no one-size-fits-all solution for fibromyalgia, but there are many natural treatments that can help lessen your symptoms. Here are 10 natural ways to treat fibromyalgia:
Rest and relaxation:
Getting enough rest is crucial for people with fibromyalgia. Taking breaks during the day and getting a good night’s sleep can help reduce fatigue and pain.
A study published in the journal Arthritis Care & Research found that people with fibromyalgia who got more than 7 hours of sleep a night reported less pain and fatigue than those who got fewer hours of sleep. Furthermore, a study published in the journal PLoS One found that people with fibromyalgia who participated in a mindfulness-based stress reduction program had reduced levels of fatigue and pain. This suggests that relaxation techniques such as yoga or meditation may help improve sleep quality and reduce fatigue and pain in people with fibromyalgia.
Exercise:
Although it may seem counterintuitive, exercise is actually one of the best things you can do for fibromyalgia. There is significant evidence to support exercise for fibromyalgia.
One study showed that a 12-week program of aerobic and resistance training improved pain, fatigue, and sleep quality in women with fibromyalgia. A review of 16 studies found that exercise was associated with significantly reduced pain intensity and improved physical function in people with fibromyalgia.
Another study showed that aquatic exercise was beneficial for reducing pain, fatigue, and improving mental health in people with fibromyalgia. Walking appears to be the most beneficial form of exercise for people with fibromyalgia, but any type of exercise that is gentle and can be sustained for a moderate amount of time is likely to be helpful. It is important to start slowly and build up gradually, listening to your body to see how much you can handle. Taking rest days when needed is also important.
Diet:
Eating a healthy diet is important for everyone, but it’s especially important for people with fibromyalgia. Some foods that are beneficial for people with fibromyalgia include omega-3 fatty acids, magnesium-rich foods, and probiotic-rich foods. One thing to avoid is trigger foods that can make symptoms worse. Common trigger foods include caffeine, alcohol, processed food, and sugar.
Supplements:
Clinical trials have shown that omega-3 supplements can be helpful for people with fibromyalgia. One study found that omega-3 supplements improved pain, fatigue, and quality of life in participants with fibromyalgia. Another study showed that omega-3 supplements reduced tenderness in the muscles of people with fibromyalgia.
Magnesium supplements have also been shown to be helpful for people with fibromyalgia. One study found that magnesium supplements improved pain and tenderness in the muscles of participants with fibromyalgia. Another study showed that magnesium supplements improved fatigue and sleep quality in participants with fibromyalgia.
Vitamin D supplements have also been shown to be helpful for people with fibromyalgia. One study found that vitamin D supplements improved pain and fatigue in participants with fibromyalgia. Another study showed that vitamin D supplements improved quality of life in participants with fibromyalgia.
Finally, turmeric supplements have been shown to be helpful for people with fibromyalgia. One study found that turmeric supplements improved pain, fatigue, and depression symptoms in participants with fibromyalgia. Be sure to talk to your doctor before starting any new supplement regimen.
Acupuncture:
Acupuncture is a traditional Chinese medicine technique that involves inserting thin needles into the skin at specific points on the body. Acupuncture has been shown to be an effective treatment for pain, fatigue, and other symptoms associated with fibromyalgia in a number of clinical trials. For example, a trial published in the journal Rheumatology International in 2012 found that acupuncture was more effective than sham acupuncture in reducing pain and fatigue in patients with fibromyalgia.
Additionally, a trial published in the journal Pain Medicine in 2013 found that acupuncture was more effective than sham acupuncture in reducing pain severity and improving function in patients with fibromyalgia. These and other clinical trials provide strong evidence that acupuncture is an effective treatment for fibromyalgia.
Massage:
Massage therapy can help relieve pain by improving circulation and relaxing tense muscles. It can also help reduce stress and promote better sleep.
Research has shown that massage therapy can be an effective treatment for pain relief in people with fibromyalgia. A study published in the journal Pain Medicine in 2016 found that massage therapy was associated with a significant reduction in pain intensity and improvement in fatigue and sleep quality in people with fibromyalgia.
Another study published in the journal BMC Complementary and Alternative Medicine in 2017 found that massage therapy was associated with a reduction in pain, anxiety, and depression symptoms in people with fibromyalgia. These findings suggest that massage therapy may be helpful for managing the symptoms of fibromyalgia.
Cannabis:
Cannabis has been shown to be an effective treatment for fibromyalgia symptoms. A 2016 study published in the Journal of Clinical Rheumatology found that cannabis was more effective than conventional therapies in treating pain, fatigue, and sleep disturbances in people with fibromyalgia. The study participants who used cannabis reported significant improvements in all measures of fibromyalgia severity, including pain intensity, fatigue, and cognitive function.
A 2017 study published in the journal Frontiers in Pharmacology found that cannabis was associated with significant reductions in pain and fatigue levels, as well as improved sleep quality. The study participants who used cannabis also reported significant improvements in quality of life.
Based on the evidence, it appears that cannabis may be an effective treatment for fibromyalgia symptoms. Cannabis is safe and easy to use, and it may provide significant relief for people who suffer from this debilitating condition.
Aromatherapy:
Aromatherapy has been shown to be beneficial for people with fibromyalgia. A study published in the journal Pain Management Nursing found that aromatherapy with lavender oil improved pain, fatigue, and sleep quality in people with fibromyalgia.
Another study published in the Journal of Alternative and Complementary Medicine found that aromatherapy with lemon balm oil improved pain, anxiety, and quality of life in people with fibromyalgia.
A study published in the International Journal of Neuroscience found that aromatherapy with bergamot oil improved pain and tenderness in people with fibromyalgia.
A study published in BMC Complementary and Alternative Medicine found that aromatherapy with chamomile oil improved anxiety and depression symptoms in people with fibromyalgia.
Laser therapy:
Laser therapy is a beneficial treatment for Fibromyalgia. It increases circulation, which helps to reduce pain and promote healing. Additionally, laser therapy is a non-invasive treatment that is relatively painless.
A study published in the “Journal of Alternative and Complementary Medicine” in 2009 found that laser therapy was able to improve pain, fatigue, and function in people with Fibromyalgia.
Additionally, a study published in “PLoS One” in 2013 found that laser therapy was able to reduce pain and improve quality of life in people with Fibromyalgia. These studies provide evidence that laser therapy may be an effective treatment for Fibromyalgia.
Intravenous vitamins and minerals:
One potential treatment for fibromyalgia is intravenous vitamin and mineral infusion. This treatment bypasses digestion and allows the vitamins and minerals to be directly absorbed into the bloodstream. The use of intravenous vitamin and mineral infusion for the treatment of fibromyalgia has been supported by a number of clinical trials.
A randomized, controlled trial published in 2011 found that the treatment was effective in reducing pain and fatigue in people with fibromyalgia. A study published in 2012 found that the infusion was associated with a significant improvement in quality of life and sleep quality.
Another study published in 2014 found that the infusion was associated with a reduction in tender points and improved self-reported pain scores. These studies provide strong evidence that intravenous vitamin and mineral infusion is an effective treatment for fibromyalgia.
Conclusion:
If you are looking for natural ways to treat Fibromyalgia, there are many options available. Some of these include: rest and relaxation techniques, exercise, diet, supplements, acupuncture, massage, cannabis, laser therapy and intravenous vitamins and minerals. It is important to speak to your naturopathic doctor about which natural therapies might be best for you. With so many options available, there is sure to be a treatment that can help improve your symptoms and quality of life.
Multiple sclerosis is a debilitating neurological disorder that can often leave patients feeling hopeless and alone. But there is hope! In this blog post, we will explore nine natural treatments for multiple sclerosis that have helped my Toronto patients alleviate some of the symptoms associated with the disease.
1. Acupuncture
Acupuncture is a traditional Chinese medicine technique that involves inserting thin needles into the skin at specific points on the body. It is believed that this helps to clear energy blockages and promote balance and healing within the body. There is some evidence to suggest that acupuncture may be effective in treating symptoms of multiple sclerosis, such as fatigue, pain, spasticity, and bladder problems.
2. Herbal Medicine
There are many different herbs that have been traditionally used to treat various ailments, including multiple sclerosis. Some of the most common herbs used for MS include ginger, ginkgo biloba, turmeric, milk thistle, lions mane and green tea. These herbs can be taken in pill form or brewed into a tea. It is important to talk to a Naturopathic Doctor or qualified herbal practitioner before starting any herbal treatment regimen, as some herbs can interact with medications you may be taking for your MS.
3. Dietary Changes
Making some simple dietary changes can also help improve symptoms of MS. One study showed that following a Mediterranean diet—which includes lots of fresh fruits and vegetables, whole grains, fish, and olive oil—may help reduce inflammation and slow the progression of MS. Other helpful dietary changes include avoiding processed foods and food allergies, getting enough vitamin D, and drinking plenty of water.
Food sensitivity testing can help to identify gluten sensitivity and other food sensitivities in people with MS and other autoimmune diseases. The most common type of food sensitivity test is an Elimination Diet, in which potential triggering foods are eliminated from the diet for a period of time and then reintroduced one at a time to see if symptoms occur. However, Elimination Diets can be difficult to stick to and can take months or even years to complete. Another option is an IgG Food Sensitivity Test, which measures levels of immunoglobulin G (IgG) antibodies in the blood.
Antibodies are produced by the immune system in response to perceived threats, such as bacteria or viruses. However, in people with food sensitivities, the immune system overreacts to harmless proteins found in certain foods, producing excessive amounts of IgG antibodies. IgG Food Sensitivity Tests can be helpful in identifying food sensitivities because they can measure levels of IgG antibodies specific to each individual food protein. This allows for a more targeted Elimination Diet and can speed up the diagnosis process. If you think you might have a food sensitivity, you can book an appointment for testing.
4. Exercise
Exercise is important for everyone, but it is especially crucial for those with MS. Regular physical activity can help reduce fatigue, improve mobility and coordination, ease depression and anxiety, promote better sleep, and boost overall fitness and well-being. Even if you are not able to do strenuous exercise due to your symptoms, there are still many low-impact activities you can do to get moving and feeling better.
5. Stress Reduction Techniques
Stress is a well-known trigger for multiple sclerosis (MS) flare-ups. Managing stress is therefore an important part of MS treatment. Stress management techniques such as relaxation therapy and yoga can be helpful, but some patients may also benefit from taking adaptogens. Adaptogens are a class of natural substances that help the body to adapt to stress by reducing the production of stress hormones. They have been used for centuries in traditional Chinese and Indian medicine, and are now gaining popularity as a natural treatment for stress and anxiety. Some common adaptogens include ashwagandha, holy basil, and ginseng. If you are interested in trying adaptogens, talk to your Naturopathic doctor first to discuss whether they are right for you.
6. Vitamin D
Vitamin D is an important nutrient that helps the body absorb calcium. It’s found naturally in very few foods, so most people get it from exposure to sunlight. Vitamin D is also available in supplement form. Some studies suggest that vitamin D may play a role in helping to prevent or treat MS. If you think you might be deficient in vitamin D, book an appointment with us for vitamin D testing or talk to your doctor.
Sometimes supplementation is ineffective or can take too long to bring up severely deficient vitamin D levels. I offer these patients the option of a high potency vitamin D injection that will bring levels up very quickly.
7. Mitochondrial Support
Mitochondrial support using resveratrol, alpha lipoic acid, coenzyme Q10 and NAD boosters is a promising new treatment for patients with multiple sclerosis. Mitochondria are the powerhouses of the cell, and they are responsible for producing energy. In patients with multiple sclerosis, the mitochondria are not working properly, and this can lead to fatigue and other symptoms. Resveratrol, alpha lipoic acid, coenzyme Q10 and NAD boosters help to support the mitochondria and improve their function. In a small study of patients with multiple sclerosis, those who received mitochondrial support had less fatigue and improved quality of life.
8. Hormones
Hormones play an important role in the human body, regulating everything from metabolism and mood to reproduction and energy levels. When hormones are out of balance, it can lead to a host of problems. For patients with multiple sclerosis (MS), hormone imbalances can cause fatigue, weight gain, depression, and loss of libido. Hormone testing can help to identify imbalances and allow for tailored treatment plans that use bio identical hormone replacement therapy to restore balance. By addressing hormone imbalances, patients with MS can improve their quality of life and potentially reduce their risk of disease progression.
9. Cannabinoids
Recently, cannabinoids have emerged as a potential therapy for MS. Cannabinoids are compounds found in the cannabis plant, and they have been shown to have anti-inflammatory and neuroprotective effects. In animal studies, cannabinoids have been shown to reduce inflammation and nerve damage in models of MS. In small clinical trials, cannabinoids have been shown to improve symptom control in patients with MS. These promising results have led to the development of several cannabinoid-based medications for MS. Dr. Shawn Meirovici N.D. is experienced cannabis educator in Toronto, Ontario. Dr. Shawn can help patients decide if cannabis therapy would be a good addition to their treatment plan.
Conclusion:
If you are living with multiple sclerosis (MS), know that you are not alone—there are millions of other people around the world dealing with this disease every day. And while there is no cure for MS at this time, there are many different treatments that can help alleviate some of the symptoms associated with the disease. In this blog post, we explored nine natural treatments for MS—acupuncture , herbal medicine , dietary changes , exercise , stress reduction techniques, vitamin D, mitochondrial support, hormone balancing and cannabinoid therapy. Make an appointment with us or talk to your doctor about which treatments might be right for you.
Intro
According to the National Sleep Foundation, “insomnia is defined as repeated difficulty with sleep initiation, maintenance, consolidation, or quality that occurs despite adequate opportunity and circumstances for rest,” and it affects approximately 30-35% of adults. If you’re one of the millions of people struggling to get a good night’s sleep, know that you’re not alone—and there are naturopathic treatments that can help!
Sleep Hygiene
One of the best things you can do to improve your sleep is to practice good sleep hygiene. This includes habits like avoiding caffeine in the afternoon and evening, avoiding alcohol before bed, Establishing a regular sleep schedule, and avoiding screens in the bedroom. Creating a relaxing bedtime routine can also be helpful; consider taking a bath or reading a book before climbing into bed.
Nutraceuticals
There are also a number of nutraceuticals—or nutrients that have medicinal properties—that can help improve sleep. Melatonin is a hormone that helps regulate the body’s natural sleep-wake cycle, and supplements can be effective in treating insomnia. 5-HTP is another nutrient that can be helpful in treating sleeplessness; it works by increasing levels of serotonin, a neurotransmitter that plays an important role in regulating sleep. Other nutrients that have been shown to be effective in treating insomnia include gamma-aminobutyric acid (GABA), valerian root, and passionflower.
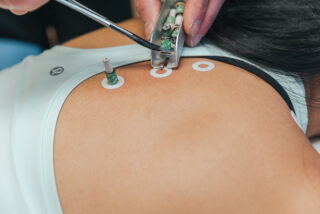
Traditional Chinese Medicine
Traditional Chinese Medicine (TCM) offers another treatment option for those struggling with insomnia. Acupuncture is one of the most well-known TCM treatments; research has shown that it can be effective in treating insomnia by promoting relaxation and improving sleep quality. Herbal medicine is another TCM modality that can be helpful in treating sleeplessness. Traditional Chinese herbs that have been used to treat insomnia include jujube seed, ziziphus seed, longan fruit, tianma root, ginseng root, and magnolia bark.
Cannabis
Cannabis is another treatment option that is gaining popularity for its ability to effectively treat insomnia. THC, the primary psychoactive compound in cannabis, has been shown to increase slow-wave sleep—the deepest stage of sleep—while CBD has been shown to reduce REM sleep density, which may lead to more restful sleep. For those who are interested in trying cannabis for their insomnia but are worried about the potential for addiction or abuse, CBD-only products may be a good option as they do not have any psychoactive effects.
Conclusion
If you’re one of the millions of people affected by insomnia, know that you’re not alone—and there are treatments out there that can help! Sleep hygiene practices like avoiding caffeine and screens before bed can make a big difference, and nutraceuticals like melatonin and 5-HTP can also be effective in treating sleeplessness. Traditional Chinese Medicine modalities like acupuncture and herbal medicine can also offer relief from insomnia; cannabis is another treatment option gaining popularity for its ability to improve sleep quality. Talk to your naturopathic doctor about which treatment option may be right for you!
Book an appointment today!
Cannabinoid therapy for sleep
I have noticed consistently good results using cannabinoids for sleep disorders. I am often asked what are the top indications for cannabis therapy in my practice and insomnia would always be in the top three.
I first started to gain an interest in cannabis and cannabinoids back in 2015. One of the most common reasons that my patients were using cannabis was for various types of insomnia. Most of these patients were having very good results. That really peaked my interest because I too suffered from insomnia for a large part of my life.
 I had used various natural sleep aids but needed a change as my current medication was producing some inconvenient side effects. After receiving my medical cannabis prescription I started using a balanced THC:CBD oil which improved my sleep latency and nighttime wakeup’s within a few days. Cannabinoid therapy is now one of my most recommended treatments for various types of insomnia as it is safe, inexpensive, fast acting and effective.
I had used various natural sleep aids but needed a change as my current medication was producing some inconvenient side effects. After receiving my medical cannabis prescription I started using a balanced THC:CBD oil which improved my sleep latency and nighttime wakeup’s within a few days. Cannabinoid therapy is now one of my most recommended treatments for various types of insomnia as it is safe, inexpensive, fast acting and effective.
Cannabis can have calming or stimulating effects depending on the preparation, dose and mode of administration. I really wanted to find out what made cannabis effective for sleep and what would be the optimal way to use it for sleep. My research pointed towards a few mechanisms through which cannabinoids likely have sleep promoting effects: GABA, Serotonin and Endocannabinoid modulation.
GABA
GABA is an inhibitory neurotransmitter that generally promotes a relaxation response in the central and peripheral nervous system. It is well established that activation of GABA receptors favours sleep and many pharmaceutical drug classes, including benzodiazepines, act on GABA receptors.
Both animal and human studies have demonstrated that cannabidiol (CBD) has a modulatory effect on GABA activity. CBD can both increase and decrease GABA activity depending on neurotransmitter activity levels (if there’s too little it increases, if there is too much it decreases). This makes CBD useful for sleep disorders resulting from too little GABA activity (think of the overactive brain) without the addictive potential of GABA stimulating pharmaceutical preparations.
Serotonin
Serotonin is a neurotransmitter that is involved in mood and sleep/wake responses. Many antidepressant medications specifically target serotonin activity. Research from the early 2000’s by Bambico et al demonstrated that cannabinoid receptor agonists (things that stimulate cannabinoid receptors) have the ability to modulate serotonin activity. Low doses seemingly to raise serotonin activity while high doses have little effect.
Both endogenous cannabinoids (cannabinoids we make ourselves) and phytocannabinoids (THC, CBD etc..) seem to have the ability to modulate serotonin activity via stimulation of our cannabinoid receptors. This may explain some of the physiology involved in the sleep promotion and anti-anxiety effects of cannabis preparations. CBD seems to be particularly useful through its interplay with our endocannabinoid system.
The Endocannabinoid System
All species, with the exception of insects, have an endocannabinoid system. The endocannabinoid system is our bodies harm reduction system, keeping chemical and electrical singling in balance. Overall, stimulation of the endocannabinoid system has a calming effect and a known modulator of our sleep/wake cycle.
 Many chronic diseases that have been linked to disruption in the endocannabinoid system (Fibromyalgia, Migraine, Inflammatory Bowel Disorder) have a sleep disruption comorbidity. This sleep disruption can usually be helped with a prescription of cannabinoids such as CBD. It is certainly plausible and empirical evidence supports the theory that patients with sleep disorders have endocannabinoid disruption. Therefore, phystocannabinoids like CBD can be helpful to restore endocannabinoid tone and subsequently better sleep.
Many chronic diseases that have been linked to disruption in the endocannabinoid system (Fibromyalgia, Migraine, Inflammatory Bowel Disorder) have a sleep disruption comorbidity. This sleep disruption can usually be helped with a prescription of cannabinoids such as CBD. It is certainly plausible and empirical evidence supports the theory that patients with sleep disorders have endocannabinoid disruption. Therefore, phystocannabinoids like CBD can be helpful to restore endocannabinoid tone and subsequently better sleep.
Dosing Considerations
Cannabis is a unique medicine as it cannot be prescribed based on age and weight. Everyone has an individual response to cannabinoids due to the fact that everyone has unique endocannabinoid tone and metabolism.
Cannabinoids like CBD and THC can interact with particular medications and preexisting conditions. Some preparations of cannabis are very different in their effect and duration. Smoked cannabis has a very fast acting effect but a short duration. Edible cannabis can have a slow onset of effect but last for a long time.
Therefore it is highly recommended to have a healthcare professional knowledgeable in cannabinoid therapy work with you for the initial stages of treatment. This will ensure a safe and effective dosing strategy with minimal chance for adverse effects. With that being said cannabis is a very safe medication and when prescribed correctly can make a significant difference in those suffering from sleep disorders. Check out the Cannabis Therapy page for more information.
References
Pretzsch CM, Freyberg J, Voinescu B, Lythgoe D, Horder J, Mendez MA, Wichers R, Ajram L, Ivin G, Heasman M, Edden RAE, Williams S, Murphy DGM, Daly E, McAlonan GM. Effects of cannabidiol on brain excitation and inhibition systems; a randomised placebo-controlled single dose trial during magnetic resonance spectroscopy in adults with and without autism spectrum disorder. Neuropsychopharmacology. 2019 Jul;44(8):1398-1405. doi: 10.1038/s41386-019-0333-8. Epub 2019 Feb 6. PMID: 30758329; PMCID: PMC6784992. Gottesmann C. GABA mechanisms and sleep. Neuroscience. 2002;111(2):231-9. doi: 10.1016/s0306-4522(02)00034-9. PMID: 11983310. Moreira FA. Serotonin, the prefrontal cortex, and the antidepressant-like effect of cannabinoids. J Neurosci. 2007 Dec 5;27(49):13369-70. doi: 10.1523/JNEUROSCI.4867-07.2007. PMID: 18057193; PMCID: PMC6673093.
The mind body connection
The mind and body are closely connected through thousands of chemical messengers. When we have a mental experience the brain sets off a cascade of neurotransmitters and hormones that affects our body. For instance when we experience joy, our body produces the hormone oxytocin. Oxytocin reduces blood pressure, stress hormone, anxiety and promotes growth and healing. Conversely, when we experience an emotion like sadness this can raise stress hormone, increasing blood pressure and eliciting negative effects on the immune system. Psychotherapy can therefore have a big impact on the health of our body by modifying mental outlook and thus inducing positive chemical messengers to the rest our body. An example is cognitive behavioural therapy, which has well documented success in the treatment of depression, anxiety and stress. https://pubmed.ncbi.nlm.nih.gov/ 31004323/
We can also treat conditions of the mind through our body. In pharmaceutical medicine, drugs like anti-depressants can block the breakdown of the neurotransmitter serotonin. Serotonin is involved in mood and therefore in some individuals boosting serotonin activity can improve mood and decrease anxiety. However, some short falls of pharmaceutical medicine is that it can often cause unwanted side effects and have a narrow therapeutic range; meaning that too little may have no effect and too much can be deadly. There are also issues with dependancy and addiction.
On the other hand nutritional and herbal supplementation can be an effective treatment for depression, stress and anxiety without the same safety concerns as drugs.
Supplementation for depression
Depression is both a physical and emotional condition. We know that depression can impact the reproductive system, immune system and our nervous system. Nutritional deficiencies can arise as a result of long standing depression and can be a precursor in the development of a depressive condition. Deficiencies in vitamin B12, vitamin D and protein are associated with depression. https://pubmed.ncbi.nlm.nih.gov/ 23377209/ In my Toronto clinic we can identify and correct nutritional deficiencies and make a big impact on depressive symptoms.
There is also a lot to be said about the impact of chronic inflammation on brain and mental health. Research has shown that chronic inflammation can increase susceptibility to depression. https:// pubmed.ncbi.nlm.nih.gov/32553197/ At the Toronto clinic we treat inflammation using supplements such as curcumin, omega-3 fatty acids and cannabidiol (CBD). These supplements can improve depressive symptoms through modulation of inflammation.
Furthermore many natural health products like CBD can also impact neurotransmitters (brain messenger chemicals) directly associated with depression. Through the interaction of cannabinoid receptors, 5-HT1A (involved in serotonin regulation) and neurogenesis factors CBD can act similarly to an anti-depressant medication but with less potential for adverse effects. At the Toronto clinic I offer cannabis education and counselling when cannabinoids would benefit a patients condition.
Supplementation for Anxiety
Anxiety disorders are the most common mental illness in the United States effecting close to 20% of the population every year. While genetics play a significant role in the development of an anxiety disorder, biological and environmental factors are pivotal as well. We know that there are often disruptions in serotonin and dopamine, cortisol and adrenaline in anxiety syndromes. A common class of drugs used in the treatment of anxiety are the benzodiazepines (Xanax, Valium, Ativan etc…). Although these medications can be very effective, they often have significant side effects (drowsiness, depression, constipation). Benzodiazepines can also be difficult to stop once started. One of the most significant mechanisms in which anti-anxiety medications work is through the GABA receptor system.
GABA is an inhibitory neurotransmitter, meaning that it helps to calm the nervous system and muscular skeletal system. Benzodiazepines have a very strong effect on GABA receptors making them effective but also potentially dangerous.
Many nutraceutical compounds activate the GABA pathway but with a gentler effect than benzodiazepines. Pharma GABA (GABA produced by bacteria), Passionflower, St. Johns Wort, Taurine, 5-HTP and CBD all have well documented effects on GABA and Serotonin. At the Toronto clinic we use these compounds successfully in the treatment of anxiety syndromes with less potential for adverse effects.https://pubmed.ncbi.nlm.nih.gov/ 11679026/
Supplementation for Stress
Every single human being experiences stress throughout their life. Stress can be a healthy natural process in the right circumstances and at the right time. Stress becomes pathological when it is experienced chronically and without appropriate instigation. Long lasting stress can have detrimental effects on multiple biological systems including the immune system, endocrine system (hormones) and cardiovascular system. https:// www.ncbi.nlm.nih.gov/pmc/articles/PMC5137920/
There are no specific pharmaceutical interventions in the treatment of stress. Benzodiazepines are the most common class of drug prescribed for debilitating stress and as I mentioned in the section on anxiety, benzodiazepines can have significant side effects and issues with dependency.
Since there is a wide spectrum of factors that can cause stress a “one size fits all” approach is not always effective. The naturopathic approach is fundamentally holistic and therefore takes into account mental, emotional and physical stressors. For instance a change in work schedule may be contributing to sleep disruption, leading to insomnia, poor work performance and nutritional disruption.
Furthermore, there is an entire class of nutritional and herbal supplements called adaptogens. Adaptogens have the ability to modulate cortisol (stress hormone) preventing peaks and dips in cortisol levels throughout the day. Overtime treatment with adaptogens facilitate a more balanced cortisol output avoiding periods of hyperactivity and burnout. To my knowledge there are no pharmaceutical drugs that act in a similar way. Some common adaptogens are: Ashwagandha, Rodiola and Siberian Ginseng. Vitamins like Vitamin C and Magnesium can help support adrenal function further helping the body to avoid burnout in periods of prolonged stress. At the Toronto clinic I use these adaptogenic compounds in conjunction with other treatments to provide a safe and effective treatment plan for chronic stress.
The mind can be treated through the body. Pharmaceutical interventions can be effective but often come with safety concerns around adverse effects and dependancy. There are many safe and effective natural approaches to mental health conditions through supplementation. At my Toronto clinic we specialize in developing an individualized plan to help achieve your mental health goals.
By: Dr. Shawn Meirovici N.D.
Intro
As a cannabis educator and naturopathic doctor I naturally get asked several questions about cannabis. Specifically cannabidiol (CBD) and epilepsy. I believe CBD enriched cannabis oil can be an effective and safe first or second line therapy for various forms of epilepsy and this is why.
Back Story on CBD and Epilepsy
Allow me to first tell you a bit about the story behind CBD and epilepsy. The potential of CBD as a therapeutic option in treating epilepsy came to the forefront back in 2013. Renowned CNN medical journalist Dr. Sanjay Gupta did a special report series on cannabis called “Weed”. One of these episodes highlighted a 5 year old girl named Charlotte Figi.
Charlotte, who had been diagnosed with a severe form of epilepsy called Dravet Syndrome, was being treated with a concentrated CBD oil. Dravet syndrome is characterized by prolonged and frequent seizures that typically begin in the first year of life. Without successful treatment, Dravet can lead to severe health concerns including developmental disabilities. After several anti-epileptic drugs failed to control her seizures, Charlottes family had began to research alternative options to help their daughter.
A little known fact is that CBD was actually discovered and researched before the most famous of the cannabinoids, delta-9 tetrahydrocannabinol (THC). Not too long after the discovery of CBD, research into the calming effects of CBD on the neurological system and its potential as an anti-epileptic came to surface.
One such study came from the Journal of Clinical Pharmacology. Published in 1981, the study found that cannabidiol was effective in almost all epileptic patients (secondary generalized epilepsy) at a dose of 200-300mg daily for 4.5 months. There were no psychological or physical symptoms suggestive of psychotropic or toxic effects. (1)
The Figi’s soon came across some of this research and began searching for high CBD strains of cannabis (not easily attainable at the time). They came across the Stanley Brothers in Colorado who had bred a high CBD low THC strain of marijuana known as “Hippie’s Disappointment”. The name suggesting its low THC content and little to no psychotropic effects.
Charlottes parents and physician said that she experienced a reduction of her epileptic seizures after her first dose of CBD oil! The strain was then renamed “Charlotte’s Web” and thus began a flurry of interest into cannibidiol and changing of marijuana laws across America.
More recently there have been several high quality clinical trials, including three phase 3 clinical trials in 2017. These trials demonstrated the efficacy of cannabidiol in reducing convulsive seizure activity; specifically in children with treatment-resistant Dravet syndrome and Lennox-Gastaut syndrome. (2)

Dr. Sanjay Gupta M.D. CNN Special Report “Weed”
How CBD works
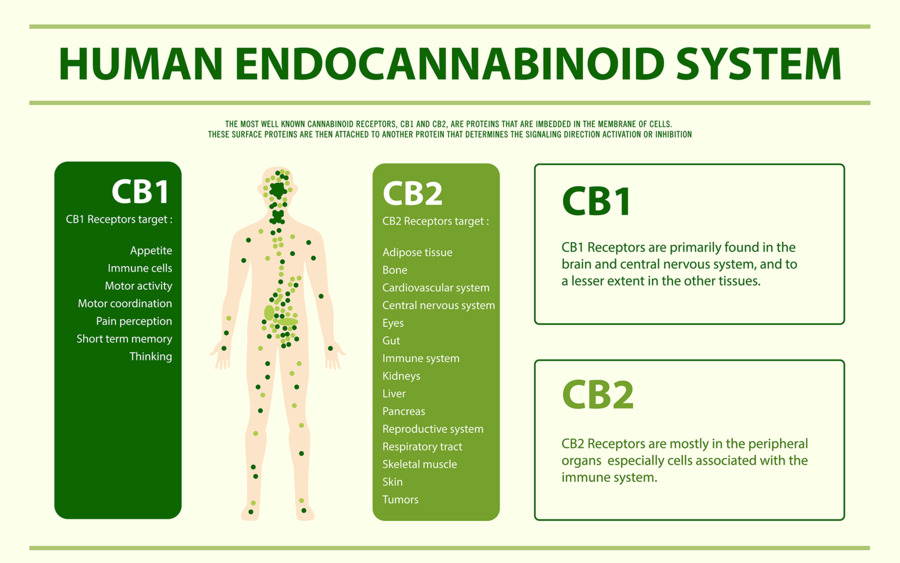
I will now explain how we think CBD works in convulsive syndromes. In order to do so I must first briefly explain an important biological system that all humans, in fact all creatures with the exception of insects, possess called the Endocannabinoid System (ECS). The ECS regulates many bodily systems to maintain balance. One such job of the ECS is to function as a self-regulating harm reduction system; essentially acting as a breaker system shutting down power when circuits get overloaded.
The ECS is able to do this via chemical messengers in our body called endocannabinoids (Cannabinoids found within our body). The two main endocannabinoids are Anandamide (AEA) and 2-Arachidonoylglycerol (2-AG). Endocannabinoids are released at the postsynaptic neuron (the receiving end of a chemical signal). Through retrograde inhibition (a feedback loop) can turn off or quiet a signal. As you can imagine, if there was no off switch things would go haywire very quickly.
Circling back to epilepsy, one of the ways the ECS functions is by maintaining homeostasis in the nervous system. The ECS is involved in the prevention of excess neuronal activity as is the case with a convulsive seizure. So you may now be wondering how CBD fits into this picture.
Our ECS is activated via receptors called cannabinoid receptors. We have many types of these receptors throughout our body. Our endocannabinoids (AEA and 2-AG) as well as phytocannabinoids (cannabinoids from plants such as THC) activate these receptors. Unlike THC, however, CBD does not fit well into our cannabinoid receptors. CBD instead boosts the activity of our endocannabinoids (AEA and 2-AG) by slowing their enzymatic breakdown.
In short, CBD can increase our endocannabinoid tone by inhibiting re-uptake. Much like how an antidepressant boosts serotonin activity by inhibiting re-uptake of serotonin.
There are many other physiological actions of CBD, such as being a potent anti inflammatory and having antidepressant effect. However, for the purposes of understanding how it can work in epilepsy, CBD is thought to act by increasing endocannabinoid tone in the nervous system.
CBD is regarded as a very safe medicinal substance as it doesn’t directly stimulate our receptors, as do many other drugs. Rather, it boosts our own innate endocannabinoid activity.

CBD Safety In Epilepsy
CBD is a generally well tolerated medication, and has no known toxicity (we’re not sure if its even possible to overdose from it). There are however some things that are important to point out to patients considering using CBD, especially when it comes to epileptic patients already taking other anti epileptic drugs (AED).
A randomized control trial (RCT) from 2018 in the journal of Neurology aimed to evaluate the safety of CBD in children with Dravet syndrome. The patients were aged 4-10 years and they received a CBD oil at relatively high doses (5, 10 or 20mg/kg/day). That equates to 65mg per day on the lower end and 260mg per day on the higher end for a 30lb child.
Considering the average adult using CBD consumes somewhere between 20-60mg per day, that’s a pretty hefty dose for a child. The results of the study indicated that for the most part CBD had no effect on other AEDs’ (Clobazam, Valproate, Levetiracetam, Topiramate and Stripentol). There was one exception with N-desmethylclobazam in which it increased levels of this drug. This effect is likely due to how CBD can slow down liver metabolism via a specific enzyme called CYP450. (3)
There was also an increase in liver enzymes in 6 patients taking both valproate and CBD. Something that may not be of much clinical significance but should be monitored. Most of my medicated patients with epilepsy are prescribed Keppra (Levetiracetam) as a first line therapy. It’s good to know that even at high doses (260mg/day) CBD is not likely to interact with this medication. Valproate is the second most common AED that I see clinically. In these patients it is recommended to test the liver enzymes every so often.
There were more adverse effects (AE) in those patients taking CBD as compared to placebo. The most common AEs’ being pyrexia, somnolence, decreased appetite, sedation, vomiting, ataxia and abnormal behaviour. In general CBD was well-tolerated. To compare, the most common AEs’ in patients taking Keppra (Levetiracetam) are: headache, increased blood pressure, somnolence, drowsiness, fatigue, anorexia, weakness, nasopharyngitis and cough. Keppra is also one of the more well tolerated AEDs’. In my opinion CBD, at the very least, is very similar to Keppra in safety profile and efficacy and should therefore be considered as a first or second line therapy.

CBD Efficacy in Epilepsy
One of the more recent studies looking into CBD and epilepsy was conducted just down the street from me at the Hospital for Sick Kids (a world renowned children’s hospital in Toronto Canada).
The study was published in the Annals of Clinical Translational Neurology in August of 2018. What was even more exciting is that the study used a CBD enriched cannabis oil from a licensed producer (Tilray) that many of my patients have access to. The CBD oil contained 100mg/ml CBD and 2mg/ml THC. Nineteen children with Dravet syndrome received the CBD oil for the complete 20-week intervention. The average dose was 13.3mg/kg/day (right in line with the dose of previously discussed safety study). The most common AEs’ were: somnolence, anorexia and diarrhea. Liver enzymes increased in patients also taking Valproate (so it looks like the interactions and adverse effects are pretty consistent).
There was a statistically significant improvement in quality of life, reduction in EEG spike activity (correlated with seizure activity), an average motor seizure reduction of 70.6% (motor seizure reduction rate in Keppra is around 37%) with a 50% responder rate of 63% (comparable to Keppra). (4)(5) Click Here for Sick Kids Study

CBD as first line therapy in Epilepsy
At this point you may be wondering why CBD is not generally considered as a first line therapy option for convulsive seizure disorders?
The reality is that the medical system in North America is generally very conservative in accepting new treatments. This is often a good thing (protecting the public from potentially dangerous or useless medications). However, on the flip side it can be a obstacle for getting naturally derived medicines, that we know to be safe and likely effective, to the patients that would benefit from them.
Currently we only have studies using CBD oil or CBD enriched cannabis oil (Containing other cannabinoids like THC) in patients with severe forms of epilepsy, or who have failed to see benefit with several other AEDs’. However, if we take into account all the information we do have on CBD, we can draw some pretty solid conclusions about its safety profile, the potential adverse effects, interactions with other drugs and its efficacy.
Until we see a robust amount of research using CBD as a first line therapy in a wider array of seizure disorders it is not likely to be accepted as a first or second or third choice by many neurologists. As a Naturopathic Doctor and cannabis educator I do see the potential of CBD for epilepsy. I will therefore continue to advocate for CBDs’ consideration as a first or second line therapeutic agent in many of my patients with epilepsy.
Check out my other articles on CBD and medical marijuana
Epilepsy Foundation stance on medical marijuana

References
- Carlini EA, Cunha JM. Hypnotic and antiepileptic effects of cannabidiol. J Clin Pharmacol. 1981;21(S1):417S-427S. doi:10.1002/j.1552-4604.1981.tb02622.x
- O’Connell, Brooke (May 1, 2017), “Cannabinoids in treatment-resistant epilepsy: A review.”, Epilepsy Behav, Epilepsy & Behavior, 70, 6, 341-348, 70: 341–348, doi:10.1016/j.yebeh.2016.11.012, PMID 28188044
- Devinsky O, Patel AD, Thiele EA, et al. Randomized, dose-ranging safety trial of cannabidiol in Dravet syndrome. Neurology. 2018;90(14):e1204-e1211. doi:10.1212/WNL.0000000000005254
- McCoy B, Wang L, Zak M, et al. A prospective open-label trial of a CBD/THC cannabis oil in dravet syndrome. Ann Clin Transl Neurol. 2018;5(9):1077-1088. Published 2018 Aug 1. doi:10.1002/acn3.621
- Abou-Khalil B. Levetiracetam in the treatment of epilepsy. Neuropsychiatr Dis Treat. 2008;4(3):507-523. doi:10.2147/ndt.s2937
By guest author: Sean Roberts
How to make cannabis butter? I am sure if you are just learning to cook with cannabis you might have several questions up your sleeves. And the good news is, you’ve come to the right place because we can help you cook cannabis butter safely from your home. You don’t require several decorated ingredients or a set of fancy cooking equipment.
All you need is simple cooking items that you can easily find in your kitchen pantry. Along with that, you will also need high-quality cannabis that you can obtain from a licenced dispensary, or directly from the producer with a medical marijuana prescription.
You don’t have to be a master chef to cook cannabis butter. However, the process requires attention, patience, and some techniques. So, jump on the bandwagon of cooking with cannabis and learn how to make cannabis butter at home.

Start With Decarboxylation Process
For beginners, the process of decarboxylation might be a little tricky. However, you will get the gist of it once you follow all the instructions given below carefully. Before we begin, here are a few things you need to learn. First and foremost, cannabis butter is a form of an edible and there are different ways of making it.
Some might avoid the decarboxylation process in order to make the butter less potent. While others look for potency in the butter. In fact, cannabis edibles are highly potent and to do so you need to first decarboxylate your cannabis. This will help you activate the psychoactive elements of the herb to its full potential.
Ideally, you have to heat cannabis at a certain temperature. The chemical reaction caused due to heating will help activate THC (psychoactive compound of the cannabis plant) and the compounds will bind together to generate the desired effect. In addition to this, you also have to take note of one more important thing. The cannabis flower contains THCA when in its raw form and this compound is non-psychoactive in nature.
Although heating causes the flower to convert THCA to THC, yet, most canna experts believe that drying cannabis before heating will help you achieve the best results. Also, keep in mind that soaking raw cannabis in heated butter will not produce the desired results. The less you soak, the better your butter will be. That said, let’s begin with the process of decarboxylation.

Things You Need To Do
You can use a microwave to decarboxylate cannabis at home. Other types of equipment that you will need include a baking tray, parchment or baking sheet, aluminum foil, and cannabis. Once you are sorted with the material, preheat your oven at 245 degrees Fahrenheit. While the oven is preheating, take a parchment paper or baking sheet and cut it to the size of your baking tray. Place the baking sheet inside the tray.
You can also keep a double layer of the aluminum foil or the baking sheet on the tray for even heat distribution. Which brings me to a very crucial scientific aspect of heating cannabis? You see, heat rises in the upward direction. Similarly, while your oven is being preheated the heat will rise in the upward direction making the oven warmer on the top and cooler at the bottom.
This means that you have to place the baking tray with dried flowers in the center of the oven in order to heat the buds at the correct temperature.
After the oven is preheated, take the tray and spread tiny pieces of cannabis on the baking sheet. Ensure that you do not break the flower into very small pieces. You can roughly break the buds into medium-sized ones to avoid the risk of over-heating or burning.
Next, place another foil paper on the top of the buds and put the tray inside the preheated oven. Bake for at least 45 minutes and once completely baked, remove it and let it cool down for another 30 minutes. Soon after cooling, you will get fresh, slightly roasted, golden-brown buds of decarboxylated cannabis ready to be infused in the butter.

How To Make Cannabis Butter?
To make cannabis butter you need to first gather a few ingredients and equipment. You will require a medium-sized saucepan, thermometer, wooden spoon, one cup of water, one cup of butter, 10 grams of decarboxylated cannabis. Next, take good quality cannabis butter in a bowl and make sure the quantity corresponds with the amount of cannabis you want to infuse in the butter.
For instance, with one cup of butter, you can use 6-8 grams of cannabis. So, make sure you infuse an optimum amount of cannabis in the butter.
For the next step, you need to take a saucepan. Put the butter using a spoon into the saucepan and add some water. Water addition is necessary because this way the butter will remain consistent. Not only this but water will prevent the bottom layer of the butter from burning or sticking to the pan. Now, turn on the gas and cook the butter in low heat.
While the butter is melting, take the decarboxylated cannabis and crush them with your hands. Add the coarsely crushed cannabis pieces into the pan containing butter and then stir it with the help of a wooden spoon. Stir until cannabis is completely soaked in the butter and cook on low heat for a maximum of two hours.
Experts believe that the ideal temperature for cooking the cannabis-infused butter is between 160-200 degrees Fahrenheit. So, check the temperature of the butter while you are cooking the mixture.
The Final Step
After two hours of stirring and cooking, turn the heat off and let the pan cool down. In the meantime, grab a cheese-cloth and a container you would want the butter to be stored in. Take the container, place a funnel on top it, and then keep the cheese-cloth over the funnel. Adjust the cloth properly and then pour the mixture over it.
Let the mixture strain into the container freely. Do not squeeze the cloth because it will allow the impurities to pass through the cloth. In case of that, you can use a spoon to create pressure on the cloth. This will allow the mixture to pass freely and the butter you get will be of high quality. After filtration, take the container and store it inside the freezer until the butter is completely ready for consumption.
About the author:

Sean Roberts is a writer by profession. He is a full time writer working with NY Marijuana Card, a leading clinic that provides medical marijuana recommendations. He aims at educating people about the medicinal use of cannabis.
My review of Ruxton by Broken Coast. Deeply relaxing, very potent 4 out of 5 stars.
My review of Aurora Cannabis MK ULTRA 4.5 stars out of 5!