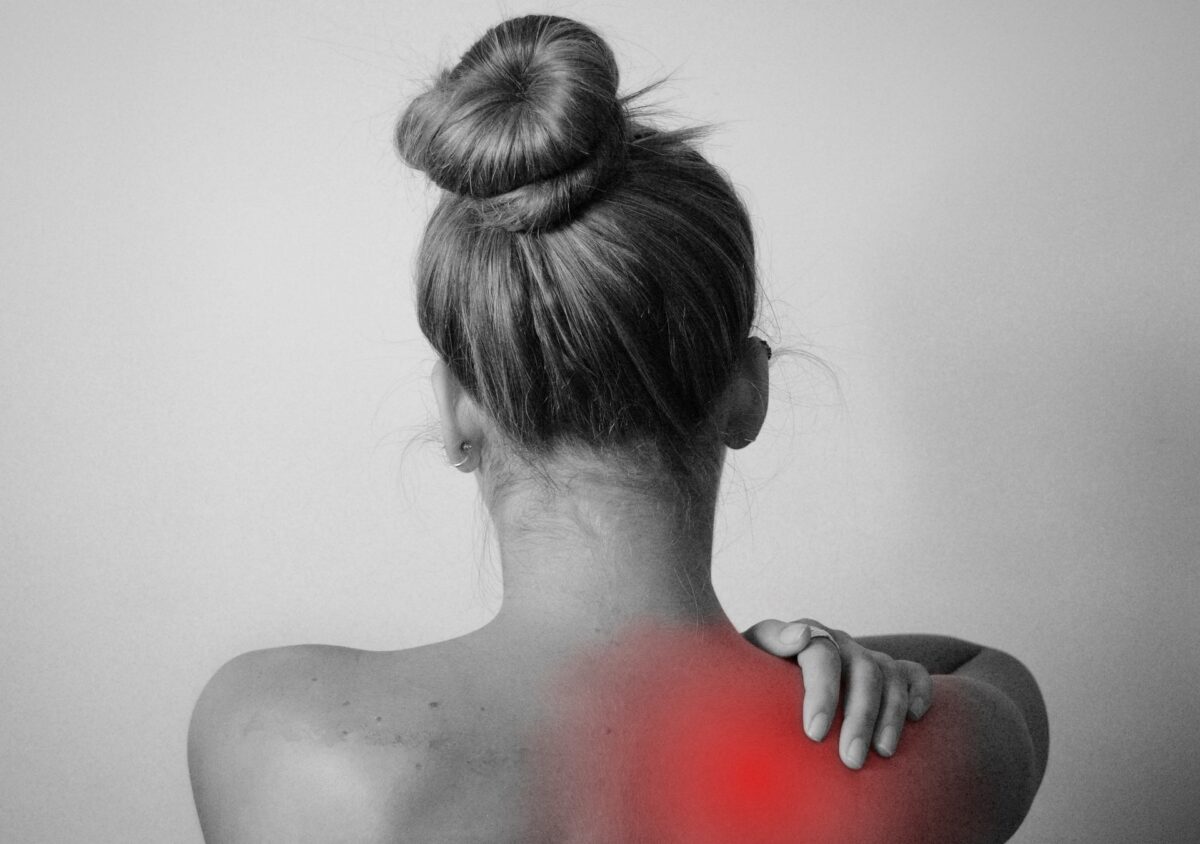
If you suffer from fibromyalgia, you know that it can be a debilitating condition that causes fatigue, pain, insomnia, gastrointestinal issues and brain fog. There is no one-size-fits-all solution for fibromyalgia, but there are many natural treatments that can help lessen your symptoms. Here are 10 natural ways to treat fibromyalgia:
Rest and relaxation:
Getting enough rest is crucial for people with fibromyalgia. Taking breaks during the day and getting a good night’s sleep can help reduce fatigue and pain.
A study published in the journal Arthritis Care & Research found that people with fibromyalgia who got more than 7 hours of sleep a night reported less pain and fatigue than those who got fewer hours of sleep. Furthermore, a study published in the journal PLoS One found that people with fibromyalgia who participated in a mindfulness-based stress reduction program had reduced levels of fatigue and pain. This suggests that relaxation techniques such as yoga or meditation may help improve sleep quality and reduce fatigue and pain in people with fibromyalgia.
Exercise:
Although it may seem counterintuitive, exercise is actually one of the best things you can do for fibromyalgia. There is significant evidence to support exercise for fibromyalgia.
One study showed that a 12-week program of aerobic and resistance training improved pain, fatigue, and sleep quality in women with fibromyalgia. A review of 16 studies found that exercise was associated with significantly reduced pain intensity and improved physical function in people with fibromyalgia.
Another study showed that aquatic exercise was beneficial for reducing pain, fatigue, and improving mental health in people with fibromyalgia. Walking appears to be the most beneficial form of exercise for people with fibromyalgia, but any type of exercise that is gentle and can be sustained for a moderate amount of time is likely to be helpful. It is important to start slowly and build up gradually, listening to your body to see how much you can handle. Taking rest days when needed is also important.
Diet:
Eating a healthy diet is important for everyone, but it’s especially important for people with fibromyalgia. Some foods that are beneficial for people with fibromyalgia include omega-3 fatty acids, magnesium-rich foods, and probiotic-rich foods. One thing to avoid is trigger foods that can make symptoms worse. Common trigger foods include caffeine, alcohol, processed food, and sugar.
Supplements:
Clinical trials have shown that omega-3 supplements can be helpful for people with fibromyalgia. One study found that omega-3 supplements improved pain, fatigue, and quality of life in participants with fibromyalgia. Another study showed that omega-3 supplements reduced tenderness in the muscles of people with fibromyalgia.
Magnesium supplements have also been shown to be helpful for people with fibromyalgia. One study found that magnesium supplements improved pain and tenderness in the muscles of participants with fibromyalgia. Another study showed that magnesium supplements improved fatigue and sleep quality in participants with fibromyalgia.
Vitamin D supplements have also been shown to be helpful for people with fibromyalgia. One study found that vitamin D supplements improved pain and fatigue in participants with fibromyalgia. Another study showed that vitamin D supplements improved quality of life in participants with fibromyalgia.
Finally, turmeric supplements have been shown to be helpful for people with fibromyalgia. One study found that turmeric supplements improved pain, fatigue, and depression symptoms in participants with fibromyalgia. Be sure to talk to your doctor before starting any new supplement regimen.
Acupuncture:
Acupuncture is a traditional Chinese medicine technique that involves inserting thin needles into the skin at specific points on the body. Acupuncture has been shown to be an effective treatment for pain, fatigue, and other symptoms associated with fibromyalgia in a number of clinical trials. For example, a trial published in the journal Rheumatology International in 2012 found that acupuncture was more effective than sham acupuncture in reducing pain and fatigue in patients with fibromyalgia.
Additionally, a trial published in the journal Pain Medicine in 2013 found that acupuncture was more effective than sham acupuncture in reducing pain severity and improving function in patients with fibromyalgia. These and other clinical trials provide strong evidence that acupuncture is an effective treatment for fibromyalgia.
Massage:
Massage therapy can help relieve pain by improving circulation and relaxing tense muscles. It can also help reduce stress and promote better sleep.
Research has shown that massage therapy can be an effective treatment for pain relief in people with fibromyalgia. A study published in the journal Pain Medicine in 2016 found that massage therapy was associated with a significant reduction in pain intensity and improvement in fatigue and sleep quality in people with fibromyalgia.
Another study published in the journal BMC Complementary and Alternative Medicine in 2017 found that massage therapy was associated with a reduction in pain, anxiety, and depression symptoms in people with fibromyalgia. These findings suggest that massage therapy may be helpful for managing the symptoms of fibromyalgia.
Cannabis:
Cannabis has been shown to be an effective treatment for fibromyalgia symptoms. A 2016 study published in the Journal of Clinical Rheumatology found that cannabis was more effective than conventional therapies in treating pain, fatigue, and sleep disturbances in people with fibromyalgia. The study participants who used cannabis reported significant improvements in all measures of fibromyalgia severity, including pain intensity, fatigue, and cognitive function.
A 2017 study published in the journal Frontiers in Pharmacology found that cannabis was associated with significant reductions in pain and fatigue levels, as well as improved sleep quality. The study participants who used cannabis also reported significant improvements in quality of life.
Based on the evidence, it appears that cannabis may be an effective treatment for fibromyalgia symptoms. Cannabis is safe and easy to use, and it may provide significant relief for people who suffer from this debilitating condition.
Aromatherapy:
Aromatherapy has been shown to be beneficial for people with fibromyalgia. A study published in the journal Pain Management Nursing found that aromatherapy with lavender oil improved pain, fatigue, and sleep quality in people with fibromyalgia.
Another study published in the Journal of Alternative and Complementary Medicine found that aromatherapy with lemon balm oil improved pain, anxiety, and quality of life in people with fibromyalgia.
A study published in the International Journal of Neuroscience found that aromatherapy with bergamot oil improved pain and tenderness in people with fibromyalgia.
A study published in BMC Complementary and Alternative Medicine found that aromatherapy with chamomile oil improved anxiety and depression symptoms in people with fibromyalgia.
Laser therapy:
Laser therapy is a beneficial treatment for Fibromyalgia. It increases circulation, which helps to reduce pain and promote healing. Additionally, laser therapy is a non-invasive treatment that is relatively painless.
A study published in the “Journal of Alternative and Complementary Medicine” in 2009 found that laser therapy was able to improve pain, fatigue, and function in people with Fibromyalgia.
Additionally, a study published in “PLoS One” in 2013 found that laser therapy was able to reduce pain and improve quality of life in people with Fibromyalgia. These studies provide evidence that laser therapy may be an effective treatment for Fibromyalgia.
Intravenous vitamins and minerals:
One potential treatment for fibromyalgia is intravenous vitamin and mineral infusion. This treatment bypasses digestion and allows the vitamins and minerals to be directly absorbed into the bloodstream. The use of intravenous vitamin and mineral infusion for the treatment of fibromyalgia has been supported by a number of clinical trials.
A randomized, controlled trial published in 2011 found that the treatment was effective in reducing pain and fatigue in people with fibromyalgia. A study published in 2012 found that the infusion was associated with a significant improvement in quality of life and sleep quality.
Another study published in 2014 found that the infusion was associated with a reduction in tender points and improved self-reported pain scores. These studies provide strong evidence that intravenous vitamin and mineral infusion is an effective treatment for fibromyalgia.
Conclusion:
If you are looking for natural ways to treat Fibromyalgia, there are many options available. Some of these include: rest and relaxation techniques, exercise, diet, supplements, acupuncture, massage, cannabis, laser therapy and intravenous vitamins and minerals. It is important to speak to your naturopathic doctor about which natural therapies might be best for you. With so many options available, there is sure to be a treatment that can help improve your symptoms and quality of life.
Cannabinoid therapy for sleep
I have noticed consistently good results using cannabinoids for sleep disorders. I am often asked what are the top indications for cannabis therapy in my practice and insomnia would always be in the top three.
I first started to gain an interest in cannabis and cannabinoids back in 2015. One of the most common reasons that my patients were using cannabis was for various types of insomnia. Most of these patients were having very good results. That really peaked my interest because I too suffered from insomnia for a large part of my life.
 I had used various natural sleep aids but needed a change as my current medication was producing some inconvenient side effects. After receiving my medical cannabis prescription I started using a balanced THC:CBD oil which improved my sleep latency and nighttime wakeup’s within a few days. Cannabinoid therapy is now one of my most recommended treatments for various types of insomnia as it is safe, inexpensive, fast acting and effective.
I had used various natural sleep aids but needed a change as my current medication was producing some inconvenient side effects. After receiving my medical cannabis prescription I started using a balanced THC:CBD oil which improved my sleep latency and nighttime wakeup’s within a few days. Cannabinoid therapy is now one of my most recommended treatments for various types of insomnia as it is safe, inexpensive, fast acting and effective.
Cannabis can have calming or stimulating effects depending on the preparation, dose and mode of administration. I really wanted to find out what made cannabis effective for sleep and what would be the optimal way to use it for sleep. My research pointed towards a few mechanisms through which cannabinoids likely have sleep promoting effects: GABA, Serotonin and Endocannabinoid modulation.
GABA
GABA is an inhibitory neurotransmitter that generally promotes a relaxation response in the central and peripheral nervous system. It is well established that activation of GABA receptors favours sleep and many pharmaceutical drug classes, including benzodiazepines, act on GABA receptors.
Both animal and human studies have demonstrated that cannabidiol (CBD) has a modulatory effect on GABA activity. CBD can both increase and decrease GABA activity depending on neurotransmitter activity levels (if there’s too little it increases, if there is too much it decreases). This makes CBD useful for sleep disorders resulting from too little GABA activity (think of the overactive brain) without the addictive potential of GABA stimulating pharmaceutical preparations.
Serotonin
Serotonin is a neurotransmitter that is involved in mood and sleep/wake responses. Many antidepressant medications specifically target serotonin activity. Research from the early 2000’s by Bambico et al demonstrated that cannabinoid receptor agonists (things that stimulate cannabinoid receptors) have the ability to modulate serotonin activity. Low doses seemingly to raise serotonin activity while high doses have little effect.
Both endogenous cannabinoids (cannabinoids we make ourselves) and phytocannabinoids (THC, CBD etc..) seem to have the ability to modulate serotonin activity via stimulation of our cannabinoid receptors. This may explain some of the physiology involved in the sleep promotion and anti-anxiety effects of cannabis preparations. CBD seems to be particularly useful through its interplay with our endocannabinoid system.
The Endocannabinoid System
All species, with the exception of insects, have an endocannabinoid system. The endocannabinoid system is our bodies harm reduction system, keeping chemical and electrical singling in balance. Overall, stimulation of the endocannabinoid system has a calming effect and a known modulator of our sleep/wake cycle.
 Many chronic diseases that have been linked to disruption in the endocannabinoid system (Fibromyalgia, Migraine, Inflammatory Bowel Disorder) have a sleep disruption comorbidity. This sleep disruption can usually be helped with a prescription of cannabinoids such as CBD. It is certainly plausible and empirical evidence supports the theory that patients with sleep disorders have endocannabinoid disruption. Therefore, phystocannabinoids like CBD can be helpful to restore endocannabinoid tone and subsequently better sleep.
Many chronic diseases that have been linked to disruption in the endocannabinoid system (Fibromyalgia, Migraine, Inflammatory Bowel Disorder) have a sleep disruption comorbidity. This sleep disruption can usually be helped with a prescription of cannabinoids such as CBD. It is certainly plausible and empirical evidence supports the theory that patients with sleep disorders have endocannabinoid disruption. Therefore, phystocannabinoids like CBD can be helpful to restore endocannabinoid tone and subsequently better sleep.
Dosing Considerations
Cannabis is a unique medicine as it cannot be prescribed based on age and weight. Everyone has an individual response to cannabinoids due to the fact that everyone has unique endocannabinoid tone and metabolism.
Cannabinoids like CBD and THC can interact with particular medications and preexisting conditions. Some preparations of cannabis are very different in their effect and duration. Smoked cannabis has a very fast acting effect but a short duration. Edible cannabis can have a slow onset of effect but last for a long time.
Therefore it is highly recommended to have a healthcare professional knowledgeable in cannabinoid therapy work with you for the initial stages of treatment. This will ensure a safe and effective dosing strategy with minimal chance for adverse effects. With that being said cannabis is a very safe medication and when prescribed correctly can make a significant difference in those suffering from sleep disorders. Check out the Cannabis Therapy page for more information.
References
Pretzsch CM, Freyberg J, Voinescu B, Lythgoe D, Horder J, Mendez MA, Wichers R, Ajram L, Ivin G, Heasman M, Edden RAE, Williams S, Murphy DGM, Daly E, McAlonan GM. Effects of cannabidiol on brain excitation and inhibition systems; a randomised placebo-controlled single dose trial during magnetic resonance spectroscopy in adults with and without autism spectrum disorder. Neuropsychopharmacology. 2019 Jul;44(8):1398-1405. doi: 10.1038/s41386-019-0333-8. Epub 2019 Feb 6. PMID: 30758329; PMCID: PMC6784992. Gottesmann C. GABA mechanisms and sleep. Neuroscience. 2002;111(2):231-9. doi: 10.1016/s0306-4522(02)00034-9. PMID: 11983310. Moreira FA. Serotonin, the prefrontal cortex, and the antidepressant-like effect of cannabinoids. J Neurosci. 2007 Dec 5;27(49):13369-70. doi: 10.1523/JNEUROSCI.4867-07.2007. PMID: 18057193; PMCID: PMC6673093.
What is Long Covid?
Long Covid is defined as symptoms that present 12 weeks after infection and that persist for at least 8 weeks. The most common symptoms being: Fatigue, Shortness of Breath and Cognitive Dysfunction. There will be an estimated 150 million cases of Long Covid cases worldwide as of 2022. Long Covid has the potential to significantly impact the lives of a large portion of the population making day to day activities difficult or near impossible. Although there are ways to reduce the risk factors in developing long covid, there aren’t many proven conventional medications to treat Long Covid once symptoms set in.
We now know that viral fragments, lingering spike protein and persistent inflammation are all likely features of Long Covid. This chronic state of immune activation leads to heart and blood vessel abnormalities, lung impairment, neurological injury and autoimmunity. Luckily, functional medicine practitioners have been at the forefront in developing protocols that work to resolve the aftermath of COVID-19 infection.
Mitochondrial Dysfunction
There is evidence of mitochondrial dysfunction in Long Covid cases as seen through disruption in fatty acid oxidation and altered lactate production. This would also partially explain the chronic fatigue of Long Covid. Functional medicine has a long history of developing protocols to address mitochondrial dysfunction. Many of the compounds used have been showing promise in treating Long Covid. For example, there is evidence of reduced levels of Coenzyme Q10 in COVID-19 infection. CoQ10 is an important compound in mitochondrial function and energy production. Supplementing with this compound along with other mitochondrial supportive nutrients (Niacin, N-Acetyl Cysteine, Alpha Lipoic Acid) have been helpful in treating Long COVID associated fatigue.
Chronic Inflammation
We also know that there is a wealth of data to suggest high levels of inflammatory markers in Long Covid sufferers. Conventionally, steroids such as prednisone have been used to effectively treat Long Covid symptoms. However, steroids can not be used indefinitely as there are significant side effects associated with long term usage. In Naturopathic and Functional Medicine we have evidence of a number of naturally derived compounds that work to treat Long Covid associated inflammation including: Curcumin, Resveratrol, Cannabinoids, Luteolin, Omega 3, and Black Cumin.
Immune System Abnormalities
We also know that there is immune system dysfunction in Long Covid as evidenced in abnormal T-cell behaviour. One of the most important compounds regulating immune function is vitamin D. There is strong evidence that having adequate vitamin D status prior to Covid infection is protective toward Long Covid and giving large doses of vitamin D to both active Covid-19 cases and Long Covid sufferers can be therapeutic.
Gastrointestinal Symptoms
Long Covid cases also seem to have a higher incidence of prolonged gastrointestinal symptoms and intestinal dysbiosis with organisms that increase inflammation. One of the best ways to treat intestinal inflammation is by promoting the growth of intestinal organisms that produce the short chain fatty acid Butyrate. Food that is high in fibre typically help to promote beneficial species of intestinal organisms. Oats, Apples, Onions, Asparagus, Broccoli, Whole grains, underripe bananas, Legumes, and Berries are some excellent foods shown to promote butyrate production.
Cannabinoids
Cannabinoids, and more specifically cannabidiol (CBD) has been shown to have some interesting mechanisms in the treatment of Long Covid. Strains of cannabis containing high levels of CBD have been shown to block spike protein from entering the cell (via ACE-2 receptors), modulate ACE-2 receptor density on cell surfaces (less doors of COVID to enter) and reduce inflammation. Therefore cannabinoids are very exciting compounds currently being investigated for use in Long Covid therapy.
Conclusions
Long Covid is a multifaceted chronic disease with effects on various physiological systems. Drugs with a narrow therapeutic scope are not going to be as effective as complex compounds that effect multiple physiological processes at the same time. This type of therapeutic synergy is a hallmark of naturally derived medicines and therefore functional medicine is going to play a pivotal role in dealing with this prevalent and highly complex disease state. In my Toronto practice I have had several cases of long covid that only began to resolve once a functional medicine protocol was put into place. So if you know someone who is suffering from Long Covid I recommend connecting them with a local Naturopathic Doctor or Functional Medicine Practitioner.
The mind body connection
The mind and body are closely connected through thousands of chemical messengers. When we have a mental experience the brain sets off a cascade of neurotransmitters and hormones that affects our body. For instance when we experience joy, our body produces the hormone oxytocin. Oxytocin reduces blood pressure, stress hormone, anxiety and promotes growth and healing. Conversely, when we experience an emotion like sadness this can raise stress hormone, increasing blood pressure and eliciting negative effects on the immune system. Psychotherapy can therefore have a big impact on the health of our body by modifying mental outlook and thus inducing positive chemical messengers to the rest our body. An example is cognitive behavioural therapy, which has well documented success in the treatment of depression, anxiety and stress. https://pubmed.ncbi.nlm.nih.gov/ 31004323/
We can also treat conditions of the mind through our body. In pharmaceutical medicine, drugs like anti-depressants can block the breakdown of the neurotransmitter serotonin. Serotonin is involved in mood and therefore in some individuals boosting serotonin activity can improve mood and decrease anxiety. However, some short falls of pharmaceutical medicine is that it can often cause unwanted side effects and have a narrow therapeutic range; meaning that too little may have no effect and too much can be deadly. There are also issues with dependancy and addiction.
On the other hand nutritional and herbal supplementation can be an effective treatment for depression, stress and anxiety without the same safety concerns as drugs.
Supplementation for depression
Depression is both a physical and emotional condition. We know that depression can impact the reproductive system, immune system and our nervous system. Nutritional deficiencies can arise as a result of long standing depression and can be a precursor in the development of a depressive condition. Deficiencies in vitamin B12, vitamin D and protein are associated with depression. https://pubmed.ncbi.nlm.nih.gov/ 23377209/ In my Toronto clinic we can identify and correct nutritional deficiencies and make a big impact on depressive symptoms.
There is also a lot to be said about the impact of chronic inflammation on brain and mental health. Research has shown that chronic inflammation can increase susceptibility to depression. https:// pubmed.ncbi.nlm.nih.gov/32553197/ At the Toronto clinic we treat inflammation using supplements such as curcumin, omega-3 fatty acids and cannabidiol (CBD). These supplements can improve depressive symptoms through modulation of inflammation.
Furthermore many natural health products like CBD can also impact neurotransmitters (brain messenger chemicals) directly associated with depression. Through the interaction of cannabinoid receptors, 5-HT1A (involved in serotonin regulation) and neurogenesis factors CBD can act similarly to an anti-depressant medication but with less potential for adverse effects. At the Toronto clinic I offer cannabis education and counselling when cannabinoids would benefit a patients condition.
Supplementation for Anxiety
Anxiety disorders are the most common mental illness in the United States effecting close to 20% of the population every year. While genetics play a significant role in the development of an anxiety disorder, biological and environmental factors are pivotal as well. We know that there are often disruptions in serotonin and dopamine, cortisol and adrenaline in anxiety syndromes. A common class of drugs used in the treatment of anxiety are the benzodiazepines (Xanax, Valium, Ativan etc…). Although these medications can be very effective, they often have significant side effects (drowsiness, depression, constipation). Benzodiazepines can also be difficult to stop once started. One of the most significant mechanisms in which anti-anxiety medications work is through the GABA receptor system.
GABA is an inhibitory neurotransmitter, meaning that it helps to calm the nervous system and muscular skeletal system. Benzodiazepines have a very strong effect on GABA receptors making them effective but also potentially dangerous.
Many nutraceutical compounds activate the GABA pathway but with a gentler effect than benzodiazepines. Pharma GABA (GABA produced by bacteria), Passionflower, St. Johns Wort, Taurine, 5-HTP and CBD all have well documented effects on GABA and Serotonin. At the Toronto clinic we use these compounds successfully in the treatment of anxiety syndromes with less potential for adverse effects.https://pubmed.ncbi.nlm.nih.gov/ 11679026/
Supplementation for Stress
Every single human being experiences stress throughout their life. Stress can be a healthy natural process in the right circumstances and at the right time. Stress becomes pathological when it is experienced chronically and without appropriate instigation. Long lasting stress can have detrimental effects on multiple biological systems including the immune system, endocrine system (hormones) and cardiovascular system. https:// www.ncbi.nlm.nih.gov/pmc/articles/PMC5137920/
There are no specific pharmaceutical interventions in the treatment of stress. Benzodiazepines are the most common class of drug prescribed for debilitating stress and as I mentioned in the section on anxiety, benzodiazepines can have significant side effects and issues with dependency.
Since there is a wide spectrum of factors that can cause stress a “one size fits all” approach is not always effective. The naturopathic approach is fundamentally holistic and therefore takes into account mental, emotional and physical stressors. For instance a change in work schedule may be contributing to sleep disruption, leading to insomnia, poor work performance and nutritional disruption.
Furthermore, there is an entire class of nutritional and herbal supplements called adaptogens. Adaptogens have the ability to modulate cortisol (stress hormone) preventing peaks and dips in cortisol levels throughout the day. Overtime treatment with adaptogens facilitate a more balanced cortisol output avoiding periods of hyperactivity and burnout. To my knowledge there are no pharmaceutical drugs that act in a similar way. Some common adaptogens are: Ashwagandha, Rodiola and Siberian Ginseng. Vitamins like Vitamin C and Magnesium can help support adrenal function further helping the body to avoid burnout in periods of prolonged stress. At the Toronto clinic I use these adaptogenic compounds in conjunction with other treatments to provide a safe and effective treatment plan for chronic stress.
The mind can be treated through the body. Pharmaceutical interventions can be effective but often come with safety concerns around adverse effects and dependancy. There are many safe and effective natural approaches to mental health conditions through supplementation. At my Toronto clinic we specialize in developing an individualized plan to help achieve your mental health goals.
Traumatic brain injury is damage to the brain that is the result of a head injury. Quality of life is greatly diminished for those living with a traumatic brain injury. Even fatal results can occur. As the quantity of study devoted to CBD develops, there is the rise in the query that whether CBD can help in treating brain injury or not. Currently, the research indicates that CBD possesses neuroprotective properties. Such effects can include mitigating the effect of head injuries.
A flexible and effective anti-inflammatory cannabinoid that has few to no adverse effects is known as cannabidiol or CBD. The number of conditions treatable with CBD increases daily with the introduction of fresh scientific information. There is emerging evidence that CBD is starting to be used as a treatment for severe traumatic brain injury.
TBI can happen to anyone who suffers from brain trauma, and it can affect every aspect of life.
What Do We Understand from Traumatic Brain Injury?
Any brain injury merits serious concern. The brain goes through a cascade of reactions after sustaining a significant injury. Inflammation, edema, and immunological activation are included in this list.
Though this is a usual and helpful set of reflexes in response to a break or fracture. Additional neurological damage might result from this set of events.
When brain cells die, the damage to the brain as a whole will soon follow. Common TBI patients include people who have served in the military, professional athletes, and victims of motor vehicle collisions. TBI can have enduring and crippling repercussions, and might manifest emotionally, physically, behaviorally, and socially.
A lot of the time, these impacts are life-altering. As well as cognitive deterioration and impaired motor function, depression and anxiety are common side effects. Severe symptoms among certain people with TBI can also result in seizures. Conventional medicine currently lacks effective treatments for minor TBI, which is an underreported and frequently misdiagnosed condition.
Scientific Evidence Which Says CBD is Effective for TBI
CBD is showing some evidence of usefulness in reducing some of the harmful effects of TBI, specifically in the areas of inflammation and neurological complications.
A paper published in Frontiers in Pharmacology claims that “The Endocannabinoid System Possesses Potentially Drugable Receptor and Enzyme Targets for the Treatment of Varying TBI Pathology.”
In addition, there are numerous studies which suggest that in combination with THC, CBD is neuroprotective, indicating that regular ingestion of cannabinoids reduces the likelihood of a catastrophic brain injury.
More and more research about TBI is becoming available with each passing year. A variety of research studies agree that the ECS plays a major role in the development of mental, bodily, and behavioral responses after a TBI.
Although further study is needed to produce precise protocols that may be accessible and recommended by mainstream medicine, some preliminary research has already been done. Each example is adding information to the outlook for the condition treated with cannabinoids.
Anecdotal Support for Using CBD as a Treatment for Brain Injury
It takes years for new scientific information to be studied and released. To draw a conclusion, you first must subject the drug being investigated, in this case CBD, to rigorous testing.
While scientific studies take time, evidence exists for the benefits of cannabis in treating brain injury based on anecdotes from patients.
CBD has the potential to improve the quality of life for people who have suffered a brain injury by allowing them to increase their quality of life.
Final Words
CBD’s brain-healing qualities are not yet fully understood and must be investigated further. Much research is being conducted regularly, and soon we will get a clearer understanding of the role of CBD in TBI. The current research suggests that CBD has some properties which can help increase quality of life in brain injury, but we cannot be sure how effective it is or if it has any side effects. We have to wait for more research to be conducted and results to be announced; only then can we be sure about how effective it is to use CBD as a treatment for brain injury.
About the author:

Sean Roberts is a writer by profession. He is a full time writer working with NY Marijuana Card, a leading clinic that provides medical marijuana recommendations. He aims at educating people about the medicinal use of cannabis https://nymarijuanacard.com/
It was my hope to find an effective alternative to Cannabidiol (CBD) that wouldn’t land me in jail when I travel; so is PEA the new CBD?
PEA stands for Palmitoylethanolamide. It is a fatty acid that is found in Eggs, Cheese, Meats and Peanuts. We also make PEA during stress, infections, inflammation, trauma, allergies, pain, cardiac disease, kidney disease and obesity. Much like our endocannabinoids, PEA is responsible for maintaining cellular homeostasis.
How does it work?
While PEA does not have a direct effect on Cannabinoid receptor (CB1 and CB2) it does have similar mechanisms of action to our endocannabinoids and cannabidiol (CBD). PEA looks very similar to our body’s own endocannabinoids (AEA and 2-AG). These similarities allow PEA to exert effects similar to our AEA and 2-AG.

PEA down regulates mast cells, which are responsible for the release of histamine and other inflammatory mediators. PEA can therefore be a powerful molecule for immune heath, inflammation, pain, neuro-protection and allergies. PEA has direct action on receptors GPCR55 and GPR119, which produce effects similar to activation of CB1 and CB2 by endocannabinoids, THC and CBD. PEA also acts similarly to CBD by affecting the breakdown of endocannabinoids via inhibition of the enzymes FAAH and MAGL.
The Research
Several studies have shown that when PEA is used with opioid type drugs for low back pain, the dose of the opioids could be reduced significantly. PEA was found to exert pain relief animal models of inflammation and neuropathic pain. These analgesic effects are thought to be due to increasing endocannabinoid levels similarly to how CBD works. All in all many studies have revealed that PEA exerts similar effects to CBD. So I thought I would give this supplement a whirl, as a alternative to CBD (especially for travel) would be an important option for patients using CBD.
My 5-day Trial with PEA
I took the supplement P.E.A. Activate from AOR , which contains 600mg PEA per lozenge. My daily dose was two lozenges per day and I did that for 5 days. I noticed a strange light-headed feeling about 5 minutes after chewing my first lozenge. The feeling lasted for a bout 30min. I was excited that I actually felt a bit different after that fist dose by unfortunately each dose produced a similar effect (a light relaxing feeling) that only lasted between 30-60min. There didn’t seem to be much carry over from one dose to another. The effects were always pretty fast acting but short-lived. Furthermore I had a return of some muscle soreness that was absent for most of the time that I was taking my CBD supplement. So, it seemed like, for me, the PEA was not having the same effect that I had experienced while on CBD.
In summary, the effects that I experienced during my PEA trial were fast acting but short-lived. PEA may therefore be a useful tool for acute episodes of anxiety, pain etc… but it did not have the same accumulative and long term effects that I experienced with CBD. The research on PEA is compelling and it is possible that this supplement warrants a more long-term trial. According to the research PEA seems to be a potential alternative to CBD but from my experience it falls a bit short. Check out my video review of PEA here.
Intro to Afghan Kush
I chose to review Pure Farms Afghan Kush because it is a best seller on the Ontario Cannabis Store and because it’s a genetically pure strain. Kush originated in Hindu Kush mountain region sandwiched between Afghanistan and Pakistan. Geographically, Afghan Kush is therefore pretty much as authentic as you can get. In fact, Pure Farms notes that this strain is the building block for many modern Kush varieties.
Pure Farms Afghan Kush is a medium to high potency Indica. The Farm is located in British Columbia. They have been cultivating for 25 years. The cannabis is grown in a modern green house facility with natural light and modern app-based quality assurance systems.

Appearance
The batch that I sampled was around 18% THC (mid-high potency) but it can land anywhere between 16-22%. When I took out my first bud I could see that it was heavily frosted with trichomes. I was also struck by the vibrant green color of the bud, which is an indication of its freshness and lack of oxidation. The texture was a bit drier than I prefer but the smoke was not harsh and very flavorful.

Smell Test
Immediately after opening the package I took a good whiff of the buds. The aroma was pleasant with definite floral and earthy notes. I knew right away that Myrcene and Linalool would be two prominent terpenes in this strain. I was able to confirm that Linalool and Myrcene were indeed part of this varieties profile, along with Nerolidol, Caryophyllene and Limonene (OCS.ca). Linalool and Myrcene are typically associated with relaxation, so I knew, even before smoking, that this would probably be a very relaxing strain.

The experience
I took 3 draws of the Afghan Kush from a joint. The effects started within 5-10 minutes and peaked around 45 minutes after smoking. The primary sensation was a nice enjoyable relaxation throughout the body and head. I would say that the body effect was not as potent as some other Indica’s that I have tried (see my review of MK Ultra). The high felt very clean and authentic, like I was transported back in time to when the first Indica strains were being cultivated. Despite the relatively high THC content there was no paranoia. I did develop a slight headache, and dizziness toward the end of the high (might have just taken a bit too much). Initially the experience wasn’t very sedating; however, towards the end I did feel quite sleepy. Therefore I would recommend this as an evening/night strain, not ideal for daytime use.
Final Thoughts
I recommend this strain to the cannabis connoisseur and those interested in trying something with a great deal of authenticity. I could also see this strain being helpful for tight sore muscles and issues with sleep and stress. Even if it was primarily a placebo effect, I enjoyed feeling connected to the roots of cannabis cultivation through this very authentic Indica.
My review of Ruxton by Broken Coast. Deeply relaxing, very potent 4 out of 5 stars.
My review of Aurora Cannabis MK ULTRA 4.5 stars out of 5!